The spine is a complex structure, comprised of nerves, connective tissue, bones, discs, muscles and other essential integrative components. Whether it getting out of a chair or car, lifting or carrying items, some 29 muscles around the pelvic girdle and lumbar spine, provide stability. In this article, we will review the anatomy of the spine, common injuries to the lumbar spine, functional assessments and training strategies to work with clients with previous injuries.

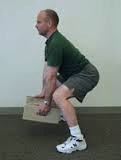
Figure 1. Sit to stand Figure 2. Lifting items
Basic Anatomy of the Spine
The spine is divided into three primary layers(internal, middle and outer).
a. Internal layer: Consists of the vertebrae of the spine, the spinal discs, and ligaments and series of small muscles that connect, one vertebra to another. The discs and ligaments perform two important functions: they stabilize the spinal column, and they provide the brain with information about the exact position of every joint and vertebra in the spine.
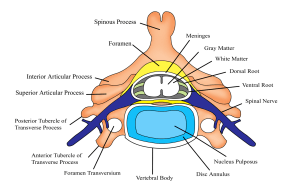
Figure 3. Internal layers of spine
b. Middle layer: There are four important muscles within the middle layer, which provide stability for the lower back. Two of these muscles comprise the back, while the other two are abdominal muscles. The muscles of the back are called the multifidus and the quadratus lumborum. The stabilizers that come from the abdominal region are called the internal oblique as well as the transverse abdominus.
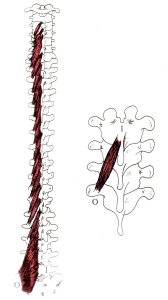
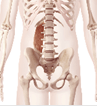
Figure 4. Multifidi Figure 5. Quadratus lumborum
c. Outer layer: This layer is the thickest. Composed of large, thick muscles, which aid in assist in transitional movements, creating and sustaining muscle contraction. The outer layer is known as erector spinae.

Figure 6. Erector spinal muscles
Biomechanics of movement
When we look at how the spine bends, flexes and rotates, there are several structures that directly produce these movements and are also affected.
Flexion and extension of lumbar spine
During lumbar flexion, the vertebrae and the intervertebral foramen in the back(posterior) separate, creating tension and stress on the posterior annulus and posterior longitudinal ligament. This forces the nucleus populous backward. Making the disc vulnerable to bulge or herniate. During extension, the opposite motion occurs. During side bending or lateral flexion, there is opening on the contralateral side and narrowing on the ipsilateral(same) side.
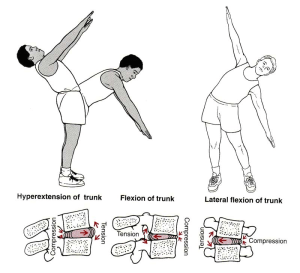
Figure 7. Source: Hamill and Knutzen
As the trunk rotates, there is tension developed in the outer annulus where the annular fibers become taught(tight). While the other half of the annular fibers slacken. At the joint, the side rotated towards approximates while the another side opens(gaps).

Figure 8. Trunk rotation
Source: Hamill and Kathleen Knutzen
Common injuries and causes of lumbar spine
There are different types of injuries the ankle can sustain. The most common are lumbar osteoarthritis(DDD), disc injuries, and spinal stenosis. In this next section, we will review
each condition providing a deeper understanding of each.
a. Lumbar osteoarthritis(DDD)
Mechanism of injury/pathophysiology: Is termed the wear and tear arthritis because it is thought that the articular cartilage breaks down because of an imbalance between mechanical stress and the ability of the joint to handle the given loads. The following are factors that can influence the development of DDD; excessive weight, repeated repetitive stressors, and muscle imbalances.
Sign and symptoms: patients will typically describe as a deep ache in the morning that eases or decreases as the day progresses. During the evening, the lower back stiffens once again.
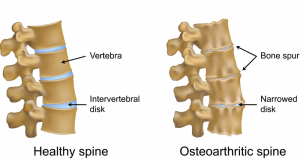
Figure 9. Lumbar degenerative changes
b. Spinal stenosis
Pathophysiology: A narrowing of the vertebral canal coupled with hypertrophy of the spinal lamina and ligament flavour or facets as the result of age-related degenerative process commonly seen in older individuals(Geenvay & Atlas 2010).
Risk Factors: Poor posture, excessive weight, muscle imbalance between flexors and extensors.
Sign and symptoms: Results in vascular compromise, bilateral pain in lower extremities particularly in back, buttocks, thighs, calves, and feet. Pain is increased with spinal extension and walking. Pain decreases with spinal flexion(bending).

Figure 10. Spinal stenosis
Medical treatment: Conservative therapies initially and if unsuccessful, decompression laminectomies may be required. In a long-term study by Atlas, S et al (2005), 148 patients,
Who either had surgery or underwent conservative care(physical therapy), were followed for 8-10 years. Results: Patients undergoing surgery had worse baseline symptoms and functional status than those initially treated nonsurgically.
c. Disc injuries
Mechanism of injury: Injury to the disc, typically occurs as a result of a combined motion such as lifting with twisting. This motion places increased stress on the disc causing an injury. Per the research and my 15 years of clinical experience, most individuals suffer from a bulging disc or herniate a disc. This is confirmed by an extensive examination by both the physician and physical therapist, an MRI, symptoms and objective findings. The four types are listed below.
Four types of disc injuries:
1. In Protrusion or bulge, there is a change in the shape of the annulus that it causes to bulge beyond its normal perimeter.
2. In Prolapse disc,(herniation), the ligamentous fibers give way, allowing the nucleus to bulge into the neural canal. The disc is still contained by the outer layers of the annulus and supporting ligamentous structures.
3 .Extrusion is where the disc protrudes through the annulus but is contained by the posterior longitudinal ligament(PLL).
4. Sequestration is where the nuclear material/free floating piece of the nucleus has partially separated from the remaining nucleus, allowing it to be free in the neural canal and moves into the epidural space.
Etiology/Risk Factors: Overstretching of the annular rings occurs as a result of a combined trunk rotation and unilateral side bending, placing the disc in a vulnerable compromised position. Repetitive compressive forces, microtrauma or one single movement at end range(flexion) with the low load will stress the posterior spinal musculature and disc.
Sign and symptoms: Loss of trunk motion/mobility, a decrease in trunk strength, central/radicular pain, possible paresthesias and painfully referred pain peripherally, inability to perform activities of daily living. Usually, worse in the sitting position or rising.

Figure 11. Disc injury
Medical treatment: During the acute stage of injury, patient education, rest, and NSAIDS are recommended. Certain positions such as flexion and combined flexion with rotation are
avoided to decrease intervertebral pressure.
Common assessments
There are several ways to assess a client with our without a spinal injury. It is important to
assess can the client maintain a neutral spine in a static position, can they maintain a neutral spine when their center of gravity is altered. Three effective assessments are the quadruped test, four point plank test, and side plank test.
1. Quadruped test
In the quadruped test, ask the client to place their hands and knees in an all fours position.
The first part(3A), as the client, to extend one leg up, hold, the repeat on another side. Then with the second part(3B), ask the client to alternate opposite arm with opposite leg. Observe if the client maintains neutral spine where the vertical arrow is, do they hyperextend their spine, excessively rotate their hips or sag?
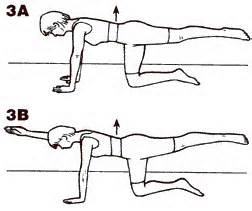
Figure 12. quadruped exercise
2. Four points (plank test)
Four point plank tests spinal erectors and paraspinal muscles.
Ask the client to assume the position in figure 13 below, prone with arms bent to 90 degrees(similar to a push-up). Then instruct the client to lift their entire body off the ground or surface while toes are in the extended position. Time them for the length of time they maintain a neutral spine(without hips sagging or spine flexing).

Figure 13. Four point bridge test
a. Grading for both tests is as follows:
Normal: Able to lift pelvis off and hold straight 15-20 second count
Good: Able to lift pelvis off but has difficulty holding spine straight for 15-20 seconds
Fair: Able to lift pelvis off but has difficulty holding spine straight for 10-15 seconds
Poor: Able to lift pelvis off but cannot hold for 1-10 seconds
Trace: Unable to lift pelvis off the table
3. Side plank test
The side plank test challenges the quadratus lumbar and external obliques.

Figure 14. Side plank test
Ask the client to position their body is in a side-lying position with the knees straight, while bending the bottom elbow at 90 degrees. Then instruct the client to lift their entire body off the ground, while keeping the legs straight. Time them for the length of time they maintain the neutral spine(without hips sagging or spine flexing).
Training strategies and programming for lumbar injuries
With any injury, the most important thing to remember is the type of injury, healing time and prior level of function of the client. Let’s begin with ankle sprains.
a. Lumbar osteoarthritis(DDD)
Recommendations for training: Joint protection, Aqua or pool therapy is an excellent intervention based upon the buoyancy principle. Closed chain exercises such as lunges, ball squats, stretching, core strengthening and aerobic exercise(ie.walking, and recumbent bicycle) are safe and effective. Particular emphasis should focus on glute and hamstring strengthening to improve sagittal stability.
b. Spinal stenosis
Recommendations for training: Anatomically and biomechanically, flexion-based exercises open the neural foramen. Perform flexion-based exercises such as; knee to chest, prayer stretch and reverse abdominal crunch. End of range extension based exercises should be avoided as they close the neural foramen (ie. cobra pressup).
Lower extremity stretching should focus stretching hamstrings, hip flexors and quadriceps. Yoga and pilates can also be effective to improve a client’s flexibility and core stability. Progressive resistance training exercises such as lat pulldown, seated mid row, seated reverse flyes, and horizontal leg press are all safe to teach a client with lumbar stenosis based on science.
c. Lumbar disc injuries
Recommendations for training: Obtain medical clearance from M.D. and communicate with client’s physical therapist prior to exercise training. Emphasis is on strengthening of “core,” abdominals, trunk muscles/lower back, and functional strengthening. Avoid combined rotational with side bending exercises, as well as hyperflexion and hyperextension motion. As these two motions place shearing forces on the disc.
Summary
The lumbar spine a complex unit that is comprised of a multitude of ligaments, tendons, connective tissue, muscles that synergistically initiate and correct movement, and stabilizes when an unstable environment. Understanding the anatomy, biomechanics and weak links
of the spine, common injuries and evidenced based training strategies, should provide you with the insight to better understand and work with clients with this kind of injuries more confidently.
Chris is the CEO of Pinnacle Training & Consulting Systems(PTCS). A continuing education company, that provides educational material in the forms of home study courses, live seminars, DVDs, webinars, articles and min books teaching in-depth, the foundation science, functional assessments and practical application behind Human Movement, that is evidenced based. Chris is both a dynamic physical therapist with 14 years experience, and a personal trainer with 17 years experience, with advanced training, has created over 10 courses, is an experienced international fitness presenter, writes for various websites and international publications, consults and teaches seminars on human movement.
REFERENCES
Atlas, S, et al, 2005, ‘Long-Term Outcomes of Surgical and Nonsurgical Management of Lumbar Spinal Stenosis: 8 to 10 Year Results from the Maine Lumbar Spine Study,’ SPINE vol. 30, number 8, pp 936–943.
Beattie, P, 2009, ‘Current Understanding of Lumbar Intervertebral Disc Degeneration: A Review With Emphasis Upon Etiology, Pathophysiology, and Lumbar Magnetic Resonance Image Findings,’ Journal of Orthopedic & Sports Physical Therapy, vol. 38, no. 6, pp. 329-337.
Colby, L, & Kisner, C, 1996, ‘Therapeutic Exercise: Foundations and Techniques,’ 3rd edition, F.A. Davis Company, Philadelphia, pp. 279-280, 431-452, 482- 508, 525, 600-618.
Genevay, S, & Atlas, S., 2010, ‘Lumbar Spinal Stenosis,’ Best Practice Residential Clinical Rheumatology, vol. 24, issue 2, pp. 253–265.
Hamill, J, & Knutzen, K, 1995, ‘Biomechanical Basis of Human Movement,’ Lippincott Williams & Wilkins, Philadelphia, pp. 16, 20, 164-165, 223-225, 289-290
Lee, D, 2004, The pelvic girdle: an approach to the examination and treatment of the lumbopelvic-hip region. 3rd edition, New York, Churchill Livingstone, pp. 48-53.
Magee, D, 1997, ‘Orthopedic Physical Assessment 3rd edition,’ W. B. Saunders Company, Philadelphia, pp. 362-366.
Oatis, C, 2004, ‘Kinesiology The Mechanics & Pathomechanics of Human Movement,’ Lippincott Williams & Wilkins, Philadelphia, pp. 8, 37-40, 45-51, 68-70, 81-88, 101-103, 113-115, 125-128, 149-150, 153, 516-520, 523-527, 776.
O’Sullivan, P, 2005, ‘Diagnosis and classification of chronic low back pain disorders: maladaptive movement and motor control impairments as the underlying mechanism,’ Journal of Manual Therapy, vol. 10, pp. 242-255.
Was this Article Helpful?
If this article was helpful to you, please consider linking this article to your own blog or sharing this through the social buttons below. You will also find other great articles at “Exercise Science“.
- 2shares
- 2Facebook
- 0Twitter
- 0Pinterest
- 0LinkedIn
- Training the Impingement Client - August 16, 2016
- Working with the older client Part 1 - May 25, 2016
- The Cervical Spine – Understanding The Science Behind Both Movement And Dysfunction - December 10, 2014


















